29th August, 2025
Heavy Periods: Causes, Symptoms & Treatment Options Every Woman Should Know
Ankura Hospital
Heavy Periods: Causes, Symptoms and Treatment Options Every Woman Should Know
Heavy periods are a common yet often overlooked women’s health concern that can signal deeper issues. From hormonal imbalances to underlying medical conditions, they can impact daily life, energy levels, and overall well-being. Wondering what’s normal, when to see a gynecologist, and how to manage it? Read on to uncover the facts about heavy menstrual bleeding.
Heavy periods are a common yet often overlooked women’s health concern that can signal deeper issues. From hormonal imbalances to underlying medical conditions, they can impact daily life, energy levels, and overall well-being. Wondering what’s normal, when to see a gynecologist, and how to manage it? Read on to uncover the facts about heavy menstrual bleeding.
A heavy period is defined as bleeding that lasts longer than 8 days or involves losing more than 80 mL of blood during a single menstrual cycle. Heavy periods, medically called menorrhagia or heavy menstrual bleeding, are a common disorder among people who menstruate, characterized by the loss of heavy blood that is typical during menstruation.
What qualifies as a heavy period?
- Having periods that last longer than seven days
- Needing to use multiple pads at a time to prevent leaking more blood
- Bleeding a lot, changing the pad or tampon every hour for several hours back-to-back
- Changing pads in the middle of the night
- Passing blood clots, the size of a quarter or larger, several times per day
- Disturbance in performing daily activities due to the period
- Abdominal pain or severe period cramps
- Feeling tired or being short of breath from losing too much blood
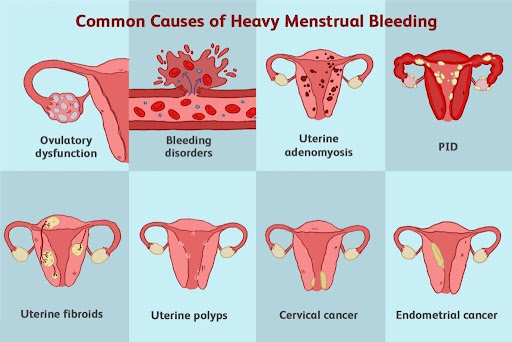
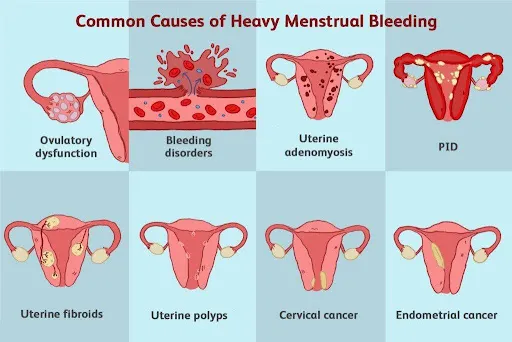
Underlying causes (fibroids, hormonal imbalance)
This condition can be caused by several factors, ranging from hormone-related issues to medical conditions or medications, such as:
Hormone imbalances
Hormone imbalances
- Anovulation
- Thyroid disease
- Polycystic ovary syndrome (PCOS)
Non-cancerous growths in uterus
- Polyps
- Fibroids
- Adenomyosis
Infection
- Chlamydia
- Gonorrhea
- Chronic endometritis
- Trichomoniasis
Pregnancy complications
- Miscarriage
- C-section niche
- Ectopic pregnancy
Other medical conditions
- Liver disease
- Kidney disease
- Pelvic inflammatory disease (PID)
- von Willebrand disease
- Leukemia or platelet disorders
Cancerous growths in your uterus
- Uterine cancer
- Cervical cancer
Medications
- Hormone replacement therapy
- Intrauterine devices (IUDs)
- Blood thinners and aspirin
- Birth control pills and injectables
Diagnosis tools (ultrasound, hysteroscopy)
- Blood tests: To check for signs of anaemia, thyroid disease, or clotting issues
- Pelvic ultrasound: A Common diagnostic tool that diagnoses menorrhagia.
- Transvaginal ultrasound: To examine the internal organs in the pelvis
- Magnetic resonance imaging (MRI): To check for abnormal structures inside the uterus when an ultrasound doesn’t provide enough information
- PAP smear: To analyze any changes in the cervix that may indicate cancer
- Cervical culture: To test for infections
- Endometrial biopsy: To check for any abnormal cells in the uterine lining or any other irregularities
Other procedures that can help the doctor to see inside and examine the vagina, cervix, and uterus to diagnose what’s the cause of bleeding, include:
- Sonohysterogram (saline–infusion sonography): To check for problems in the lining of the uterus.
- Hysteroscopy: To check for fibroids, polyps, or other irregular tissue in the uterus.
Medical and surgical treatments
Treatment varies based on cause, severity, age, medical history, and health condition. However, in some cases, menorrhagia gets better without needing treatment. Medications Before recommending surgical treatments, doctors suggest medications, such as
- Iron supplements: To improve the iron levels
- Nonsteroidal anti-inflammatory drugs (NSAIDs): To ease the cramps and reduce the bleeding.
- Antifibrinolytic medicines: To prevent clots from breaking down and causing excessive bleeding.
- Birth control: These include pills, patches, coils, vaginal rings, and IUDs, which help to regularize the periods and lighten the blood flow.
- Hormone replacement therapy (HRT): To help balance the hormonal (estrogen and progesterone) levels in the body to reduce heavy periods.
- Gonadotropin-releasing hormone (GnRH) agonists and antagonists: To stop or reduce the bleeding temporarily
- Desmopressin nasal spray: To stop bleeding associated with von Willebrand disease by helping the blood clot
Surgical treatments If medication doesn’t improve the symptoms, the doctor recommends a minor surgical procedure, such as:
- Hysteroscopy: This procedure is performed to diagnose and treat heavy bleeding, using a thin, lighted tube to see inside the uterus.
- Myomectomy: This procedure is used to remove fibroids from the uterus.
- Hysterectomy: This procedure is performed to remove the uterus and prevent having periods or pregnancy.
- Uterine artery embolization (UAE): This is the procedure that is performed to restrict the blood flow from fibroids and tumours.
- Endometrial ablation: This procedure is performed to destroy all or part of the uterine lining.
- Dilation and curettage (D&C): This procedure is performed to remove the outermost layer of the uterine lining and sends the tissue to a lab to detect the cause.
Lifestyle and dietary tips
- Get Regular Exercise
- Manage Stress
- Get Enough Sleep
- Monitor Your Cycle
- Eat Iron-Rich Foods
- Boost Iron Absorption
- Stay Hydrated
- Limit Caffeine and Processed Foods
Conclusion
Heavy periods (menorrhagia) can result from hormonal imbalances, uterine conditions, or underlying health issues. If you’re experiencing prolonged or excessive bleeding, it’s important to consult a gynecologist. Treatment options range from medications to surgical procedures. Lifestyle changes and a balanced diet can also help manage symptoms.
Related Specialties
Frequently Asked Questions
Our healthcare specialists are equipped with the knowledge and skills to provide you with the support you require. From consultation to diagnosis to treatments, our experts are dedicated to helping you.